FDA Brief, Week of September 21, 2015
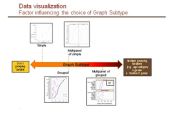
Seeing is believing: Making clinical trial statistical data from medical product testing easy to understand
- Trick to tell clear, compelling stories – Creating tables and graphs that aren’t dense
- Tool for Public from Safety Graphics Working Group : Web-based, step by step process for graphical designs for reporting clinical trial safety data
- Designs clearly illustrate statistical data representing a wide variety of adverse effects observed during clinical trials or post-approval
Strengthening the Clinical Trial Enterprise for Medical Devices: An FDA/CDRH Strategic Priority Update
- Clinical trial data are required in premarket submissions for the highest risk devices : To demonstrate reasonable assurance of safety and effectiveness,
- FDA Objective : Reducing the time and cost of regulatory and non-regulatory aspects of the U.S. clinical trial enterprise, while assuring the protection of human subjects and the generation of robust data.
- New Guidances : benefits and risks for Investigational Device Exemptions (IDEs) decisions, . adaptive designs
- Early Feasibility Studies (EFS) program encouraged : Small clinical studies to gain early insights into an innovative technology during the development process before starting a larger clinical trial.
FDA’s Patient Preference Initiative: The Need for Evolving Tools and Policies
FDA launched Patient Engagement Advisory Committee – see in ‘What To Watch’. Additional perspectives:
- Patient preference Initiative launched in 2013 : Captures patient-centered perspectives in its structured benefit-risk framework, for device evaluation and approvals
- Device product labeling could include description of patient preferences to make well-informed decisions.
- Better tools needed to accurately capture and characterize patient views on acceptable balances of benefits and risks
- Draft Guidance will help device-makers assess patient valuations of benefit and risk related to relevant device types, illnesses, and conditions
- Better understanding of patients’ experiences, needs, and views, will improve product development and enhance the safe and effective use
LONSURF ( trifluridine and tipiracil, Taiho Oncology, Princeton, NJ)
Description : Contains thymidine-based nucleoside analog, trifluridine, and the thymidine phosphorylase inhibitor, tipiracil. Tipiracil increases trifluridine exposure by inhibiting its metabolism by thymidine phosphorylase. Following uptake into cancer cells, trifluridine is incorporated into DNA, interferes with DNA synthesis and inhibits cell proliferation.
Indication: Treatment of metastatic colorectal cancer who have been previously treated with fluoropyrimidine-, oxaliplatin- and irinotecan-based chemotherapy, an anti-VEGF biological therapy, and if RAS wild-type, an anti-EGFR therapy.
Efficacy: Single randomized, double-blind, placebo-controlled study conducted in patients with previously treated metastatic colorectal cancer, n= 800, LONSURF (N=534) plus best supportive care (BSC) vs placebo (N=266) plus BSC
- Statistically significant improvement in overall survival (p,0.001) and progression-free survival (p<0.001) were demonstrated in patients
Safety: Anemia, Neutropenia, Thrombocytopenia, physical weakness, fatigue, decreased appetite, diarrhea, vomiting, abdominal pain and fever.